Science is uncovering a surprising relationship between our gut and our brain. For decades, depression has been considered a strictly neurological disease, but recent research reveals that the state of our gut microbiota could be a key factor in its development and treatment.
How Does the Microbiota Affect Our Mental Health?
Our gut harbors billions of microorganisms that play essential roles, such as producing vitamins, modulating the immune system, and regulating metabolism. But that’s not all: this microbial community also influences our mood through the microbiota-gut-brain axis.
The Vagus Nerve and Its Role in Gut-Brain Communication
The vagus nerve is an information highway that directly connects the digestive tract with the brain. Through it, neurochemical signals travel in both directions, allowing the brain to regulate digestive functions while simultaneously receiving information about the gut’s condition.
When gut microbiota is balanced, the vagus nerve helps maintain an appropriate stress response and stable emotional regulation. However, if the microbiota is disrupted, negative signals may be sent to the brain, promoting anxiety, depression, and sleep disturbances. Recent studies have shown that vagus nerve stimulation can improve depressive symptoms, reinforcing the idea that the gut and brain are deeply interconnected.
The Immune System and Its Relationship with Brain Inflammation
The gut is not just a digestive organ; it is also a key component of the immune system. Under normal conditions, gut microbiota helps regulate inflammation, preventing excessive immune responses that could harm the body.
However, when microbiota is imbalanced due to stress, an unhealthy diet, or excessive antibiotic use, the intestinal barrier can become permeable. This allows bacterial toxins to enter the bloodstream, triggering systemic inflammation that can reach the brain. Chronic inflammation has been strongly linked to neuropsychiatric disorders such as depression and anxiety because it interferes with the production of essential neurotransmitters like serotonin and dopamine.
Microbial Metabolites and Neurotransmitter Production
Gut microorganisms not only process the food we eat but also produce metabolites that can directly influence brain chemistry. Among them, short-chain fatty acids (SCFAs) stand out, as they strengthen the blood-brain barrier and reduce oxidative stress, thus supporting neuronal protection.
Additionally, gut microbiota plays a crucial role in the production of key neurotransmitters such as serotonin and gamma-aminobutyric acid (GABA). It is estimated that 90% of the body’s serotonin is produced in the gut thanks to the presence of certain beneficial bacteria. Serotonin is fundamental for mood regulation, sleep, and overall well-being, so a disrupted microbiota can influence the development of emotional disorders.
GABA, in turn, is an inhibitory neurotransmitter that reduces neuronal excitability and helps control anxiety. Research has found that certain species of Lactobacillus and Bifidobacterium can increase GABA production, suggesting that microbiota manipulation through probiotics could be a therapeutic strategy for disorders like anxiety and depression.
Probiotics and Prebiotics: Allies for the Brain
Research has shown that probiotics (live beneficial bacteria) and prebiotics (fiber and nutrients that feed microbiota) can improve mental health. Animal studies have shown that certain strains of Lactobacillus and Bifidobacterium can reduce anxious and depressive behaviors. In humans, probiotic supplementation has shown modest antidepressant effects, although more studies in clinical populations are needed.
Probiotic-rich foods such as yogurt, kefir, kimchi, and sauerkraut can help maintain microbiota balance, while prebiotics found in foods like garlic, onions, asparagus, and oats promote the growth of beneficial bacteria.
Additionally, certain fermented foods can influence the production of short-chain fatty acids, which contribute to intestinal barrier integrity and, consequently, reduced gut permeability. This is crucial since increased permeability can lead to systemic inflammation, which is closely linked to mood disorders.
Inflammation and Depression: An Unexpected Connection
Studies have found that many people with depression have elevated levels of inflammation in their bodies. A disrupted microbiota can contribute to this inflammation by allowing bacterial toxins to enter the bloodstream. In this context, probiotics can act as anti-inflammatory agents, helping restore gut homeostasis and reducing depressive symptoms.
Furthermore, some gut bacteria can modulate the production of inflammatory cytokines and reduce oxidative stress—two key factors in neuroinflammation associated with depression. Chronic inflammation, in addition to its impact on mental health, also affects metabolic regulation. It has been observed that it can contribute to insulin resistance and metabolic dysfunction, highlighting the importance of maintaining a balanced microbiota. This link between inflammation, metabolism, and mental health underscores the need for integrated strategies to address these issues holistically.
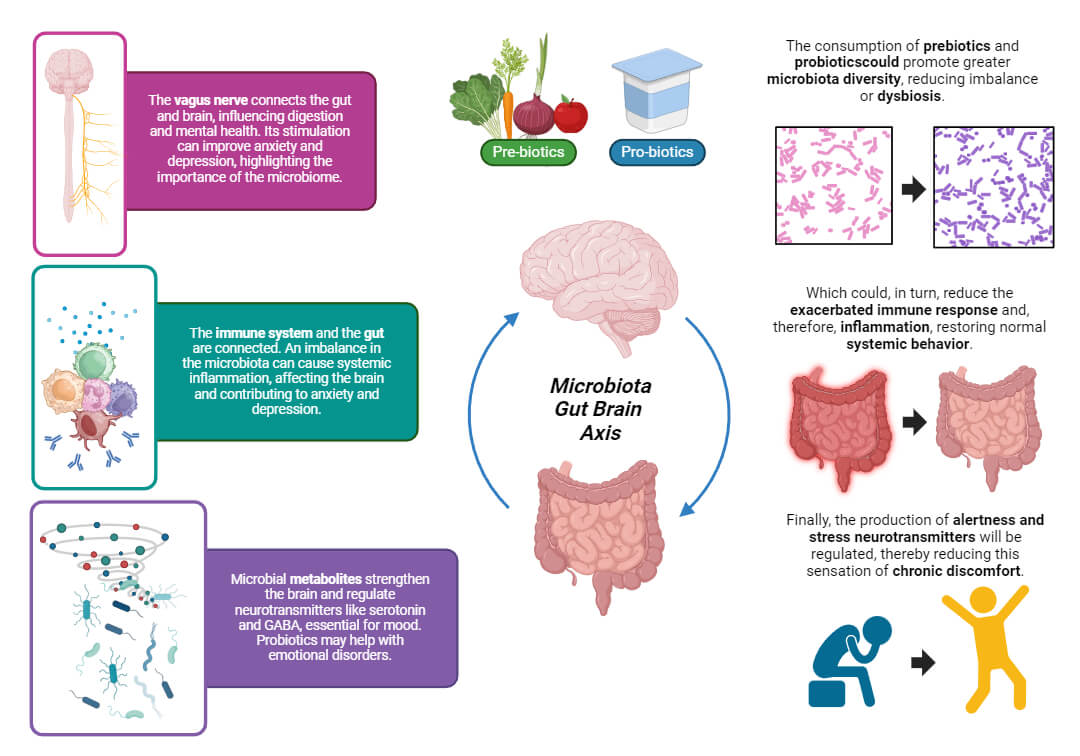
Figure 1. Mechanism of gut microbiota regulation in immune response, neurotransmitter production, and its impact on stress, anxiety, and depression.
The Future of Depression Treatment?
Despite advancements, research in this field is still in its early stages. While the results are promising, large-scale studies with rigorous methodologies are essential to confirm the therapeutic role of probiotics and prebiotics in mental health. Nevertheless, maintaining a balanced microbiota through a fiber-rich diet, fermented foods, and avoiding excessive antibiotic use could be a complementary strategy to improve mental well-being.
Future research may even lead to the development of psychobiotics—probiotics specifically designed to modulate the microbiota-gut-brain axis and enhance mood. These developments could represent an alternative or complement to traditional treatments for depression and anxiety, offering a more holistic approach to mental health.
Conclusion
The connection between gut microbiota and the brain is revolutionizing our understanding of mental health. Although much remains to be discovered, it is clear that a healthy gut can be an important key to a healthy brain. As science advances, we may be on the verge of a new era in the treatment of mood disorders, where nutrition and microbiota play a leading role.
Taking care of our microbiota not only benefits digestive health but could also become an essential tool for improving mental health and overall quality of life. Adopting healthy habits, reducing stress, and consuming foods that promote bacterial diversity could be simple yet powerful strategies for maintaining physical and emotional well-being.
Main Reference:
Radford-Smith, D. E., & Anthony, D. C. (2023). Prebiotic and Probiotic Modulation of the Microbiota–Gut–Brain Axis in Depression. Nutrients, 15(8), 1880. https://doi.org/10.3390/nu15081880
Other References:
Cryan, J. F., O’Riordan, K. J., Cowan, C. S. M., Sandhu, K. V., Bastiaanssen, T. F. S., Boehme, M., Codagnone, M. G., Cussotto, S., Fulling, C., Golubeva, A. V., Guzzetta, K. E., Jaggar, M., Long-Smith, C. M., Lyte, J. M., Martin, J. A., Molinero-Perez, A., Moloney, G., Morelli, E., Morillas, E., O’Connor, R., … Dinan, T. G. (2019). The Microbiota-Gut-Brain Axis. Physiological reviews, 99(4), 1877–2013. https://doi.org/10.1152/physrev.00018.2018
Sarkar, A., Lehto, S. M., Harty, S., Dinan, T. G., Cryan, J. F., & Burnet, P. W. (2016). Psychobiotics and the manipulation of bacteria–gut–brain signals. Trends in neurosciences, 39(11), 763-781.
Gibson, G. R., Hutkins, R., Sanders, M. E., Prescott, S. L., Reimer, R. A., Salminen, S. J., … & Reid, G. (2017). Expert consensus document: The International Scientific Association for Probiotics and Prebiotics (ISAPP) consensus statement on the definition and scope of prebiotics. Nature reviews Gastroenterology & hepatology, 14(8), 491-502.


