One of the most silent yet deeply debilitating symptoms in patients with advanced cancer is apathy: that complete loss of motivation that leads to no longer eating, moving, or even wanting to keep fighting. Traditionally, this lack of drive has been considered simply the result of physical or emotional exhaustion. However, a recent study published in Science shows that this lack of willpower is not just a psychological reaction (it’s a direct consequence of inflammatory processes that affect the brain). In other words, apathy is also biological.
This study focused on cachexia, a complex syndrome commonly seen in patients with late-stage cancer. Cachexia is not just about weight loss. It involves a severe decrease in muscle mass, appetite, energy, and in many cases, also the desire to act. It is estimated that more than 50% of patients with advanced cancer develop cachexia, making it one of the leading causes of functional decline and death, even when the tumor itself has not yet reached a critical size.
What the researchers discovered is that this demotivation doesn’t simply occur because the body is weak, but because the immune system (when detecting the presence of cancer) produces a molecule called interleukin-6 (IL-6). This substance is a proinflammatory cytokine, meaning a signal released by the body during chronic illness or immune activation. IL-6 travels to a region of the brain known as the area postrema, which acts like a “surveillance zone” that detects changes in the bloodstream and communicates this to the rest of the brain.
From there, the inflammatory signal moves to the lateral parabrachial nucleus, a region that integrates bodily signals to regulate responses such as pain, appetite, and defense behaviors. This area then influences deeper regions of the brain, including the substantia nigra and the nucleus accumbens, which are key parts of the dopaminergic system the circuit responsible for regulating motivation, reward, and goal-directed behavior.
The end result of this cascade is a significant reduction in dopamine. And when there’s less dopamine circulating, the brain simply stops sending the signals that normally make us seek rewards or stay active. In cancer patients, this translates into a profound loss of desire to eat, engage socially, follow treatments, or even get out of bed.
This mechanism, in fact, has evolutionary roots. In acute inflammation (such as during an infection or injury) this neuroimmune pathway serves an adaptive purpose: it reduces physical activity so the body can conserve energy and focus on healing. However, in the context of chronic diseases like cancer, where inflammation persists over long periods, this same mechanism becomes harmful, as it promotes a sustained state of demotivation that further worsens the patient’s condition.
What’s most remarkable is that this process is reversible. In animal models, the researchers were able to restore the animals’ motivation by blocking IL-6 with specific antibodies. They also managed to reactivate normal behavior by interfering with the brain connections transmitting these inflammatory signals, or by stimulating dopamine production. In all cases, the animals resumed goal-directed behaviors like seeking food and engaging with their environment.
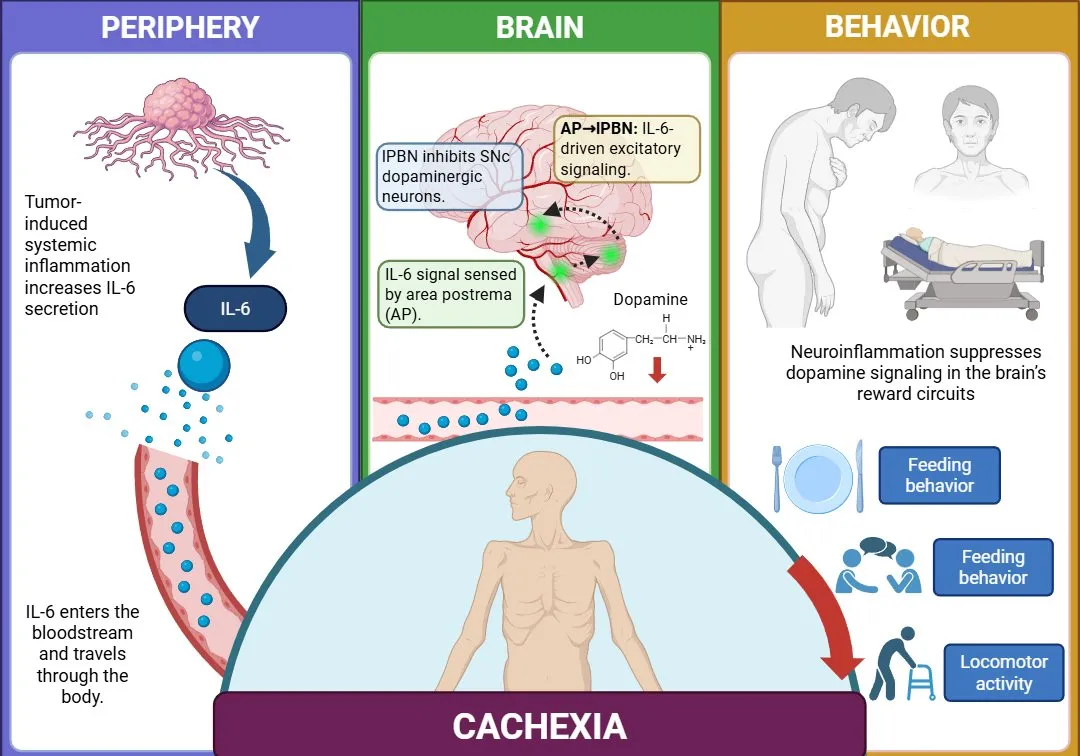
Figure 1. Cancer-induced inflammation activates a brain circuit that reduces dopamine and suppresses motivation, contributing to behavioral symptoms of cachexia such as loss of appetite and physical activity.
These results open new doors for medicine. Traditionally, the approach to cachexia has focused on countering muscle loss through nutrition or anabolic agents. But if part of the problem lies in the brain (in how inflammation modulates motivation) then we need to complement physical strategies with interventions that restore the patient’s will to act.
This finding also reminds us that not all apathy is emotional. In cancer patients, the lack of desire to keep going is not always a matter of mindset or attitude — it can be the biological effect of a very real signal altering brain chemistry. And most importantly: that signal can be interrupted.
Understanding that the immune and nervous systems are deeply connected is key to designing truly integrative therapies. Treating cancer is not only about destroying tumor cells, but also about restoring essential functions of both body and mind, including the motivation to live.
Because in the end, the will to live is also a biological function.
And science is finding ways to bring it back.
Main reference:
Zhu, X. A., Starosta, S., Ferrer, M., Hou, J., Chevy, Q., Lucantonio, F., Muñoz-Castañeda, R., Zhang, F., Zang, K., Zhao, X., Fiocchi, F. R., Bergstrom, M., Siebels, A. A., Upin, T., Wulf, M., Evans, S., Kravitz, A. V., Osten, P., Janowitz, T., … Kepecs, A. (2025). A neuroimmune circuit mediates cancer cachexia-associated apathy. Science (New York, N.Y.), 388(6743), eadm8857. https://doi.org/10.1126/science.adm8857
Other reference:
Melero, I., de Miguel Luken, M., de Velasco, G. et al. Neutralizing GDF-15 can overcome anti-PD-1 and anti-PD-L1 resistance in solid tumours. Nature 637, 1218–1227 (2025). https://doi.org/10.1038/s41586-024-08305-z
Evans, W. J., Morley, J. E., Argilés, J., Bales, C., Baracos, V., Guttridge, D., Jatoi, A., Kalantar-Zadeh, K., Lochs, H., Mantovani, G., Marks, D., Mitch, W. E., Muscaritoli, M., Najand, A., Ponikowski, P., Rossi Fanelli, F., Schambelan, M., Schols, A., Schuster, M., Thomas, D., … Anker, S. D. (2008). Cachexia: a new definition. Clinical nutrition (Edinburgh, Scotland), 27(6), 793–799. https://doi.org/10.1016/j.clnu.2008.06.013
Fearon, K., Strasser, F., Anker, S. D., Bosaeus, I., Bruera, E., Fainsinger, R. L., Jatoi, A., Loprinzi, C., MacDonald, N., Mantovani, G., Davis, M., Muscaritoli, M., Ottery, F., Radbruch, L., Ravasco, P., Walsh, D., Wilcock, A., Kaasa, S., & Baracos, V. E. (2011). Definition and classification of cancer cachexia: an international consensus. The Lancet. Oncology, 12(5), 489–495. https://doi.org/10.1016/S1470-2045(10)70218-7


